The Opioid Epidemic: Facts and Remedies
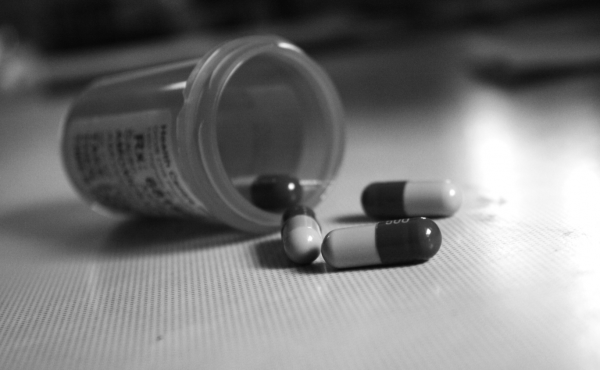
In 2007, 14.6 percent of U.S. college students have used prescription drugs nonmedically. (Photo Via Flickr)
September 26, 2018
Opiate addictions date back to antiquity when the ancient Egyptians, Persians and Chinese used poppy plant extract as mood relaxers. In the mid-19th century, Great Britain orchestrated an opium addiction epidemic in China. The lucrative trade strategy involved the British introducing Indian opium to China. Shortly after, a large percentage of the Chinese population became addicted. This allowed the British to trade Indian opium for tea, porcelain and silks, while keeping their silver reserves intact.
Opiates were exploited and weaponized to work against nations because of their addictive qualities. Today, these attributes of opium are detrimentally impacting our loved ones and peers.
Opioids are opiate derivatives that are synthetically manufactured to act as pain relievers. Unfortunately, because of their inherently addictive nature and lethal consequences, millions of American lives have been lost to the substance. According to reports from U.S Department of Health and Human Services (HHS), 115 individuals die every day because of opioid overdoses. Annually, 11.5 million people misuse prescription opioids and just under 1 million people use heroin. 40 percent of the 42,000 deaths from opioid overdose were due to commonly prescribed sedatives. The opioid crisis also put a $504 billion dent in the U.S. economy owing to costs associated with treatment.
Opioids gained popularity towards the end of the 19th century in the U.S. when pharmaceutical companies endorsed the drug with falsified reports suggesting that these pain relievers were not addictive. Following these claims, doctors increasingly prescribed opioids to mitigate discomfort. Not long after the mass distribution of the drugs was it realized how addictive opioids actually are. Individuals were seen misusing and abusing prescription variants of the drug including heroin, vicodin, oxycodone, methadone, fentanyl and morphine. The addictive qualities of opioids make ordinary people susceptible to abuse and overdose. Some even turn to heroin if they do not have access to prescription drugs.
To understand why opioids are so addictive, it is important to know how they work. We all have endogenous opioids in our body that attach to receptors in our brain when we encounter pain. These naturally occurring opioids cannot be produced in high numbers so doctors prescribe synthetic opioids to alleviate chronic pain. After attaching to receptors in the brain, synthetic opioids signal the brain to flood the circuit with dopamine, a neurotransmitter that produces euphoric effects. This reaction allows the brain to assuage any distressing feelings by enforcing a calming effect.
The physiology of our brain ensures we repeat behaviors that reward us. When one is using opioids, they are being rewarded with the overstimulation of their system due to increased levels of dopamine. Without their knowledge or understanding, individuals will repeat these drug-seeking behaviors which they think will reproduce rewarding results, leading to the unintentional misuse and abuse of drugs.
According to Patrice Malone M.D., of Columbia University and New York State Psychiatric Institute, college students have increased their use of opiates in the past 20 years which subsequently led to many accidental overdoses. Opioid consumption by college students increased by 343 percent from 1993 to 2005. Research also indicates that students who consume prescription opioids without medical supervision tend to exhibit other “risky behaviors,” which increases their likelihood of overdose. In 2007, 14.6 percent of U.S. college students have used prescription drugs nonmedically. When used in conjunction with other drugs, the likelihood of overdose is far more prevalent. Although the prescription rate for opioids has fallen since its peak in 2010, college students annually fall victim to opioid abuse.
In 2017, President Donald Trump declared the opioid epidemic a national crisis prompting the HHS to assess the severity of the epidemic and to create a plan to combat the public health emergency.
Many national public health leaders came forward with ideas and strategies about how to deal with the opioid crisis. Anne Constantino, CEO of Horizon Health Services, proposed implementing a massive educational campaign to make the information about the risks of addiction more accessible to vulnerable communities. Richard Blondell, M.D., of the National Center for Physician Training in Addiction Medicine, suggested making it a part of the education system and bring awareness to addiction at younger ages. Blondell also recommended that Congress enact legislation that mandates doctors to learn about addiction before they are given a Drug Enforcement Administration license to prescribe addictive drugs.
Osmond Quiah, M.D., chief of the Medically Managed Detoxification Unit at Woodhull Medical Center and affiliate of NYU Langone Medical Center, emphasized that doctors are aware of the various medications that are addictive and they understand how doses have to be controlled and monitored. Nonetheless, he urged the importance of continued training from the moment physicians complete their residency to the time they choose to retire. Kevin Kunz M.D., executive vice president of the Addiction Medicine Foundation, said that although the majority of medical schools do offer education about opioids, only eight percent teach about the topic of addiction. There are also very few mandatory workshops pertaining to addiction for medical doctors.
Nevertheless, physicians are making efforts to curtail the prevalence of opioids by using other narcotics such as Suboxone and Methadone to curb addiction as well as supplementing non-narcotic intervention plans to create additional treatment options.
The efficacy of opioids as pain relievers is undeniable. Though they have addictive qualities, opioids fulfill the purpose they were created for. It is injudicious to impose a ban on them, but it is important to limit them. “When there is genuine pain, no one should suffer. Especially patients who are terminally ill, have suffered from a severe accident, have war trauma or are under post-operative care,” Quiah said, adding that “treatment is essential for our patients, but addiction prevention is a key component to effectively resolve this crisis.”